Sudden Decline in Maternal Mortality During Pandemic Related to Assault, Accidents
The maternal mortality rate is regularly considered a black eye for the American health care system. The number of deaths of mothers surrounding labor is distinctly high for a developed nation like the U.S. Internationally, it ranks near less developed second-world countries like Uzbekistan, Moldova, and Uruguay based on World Bank data.
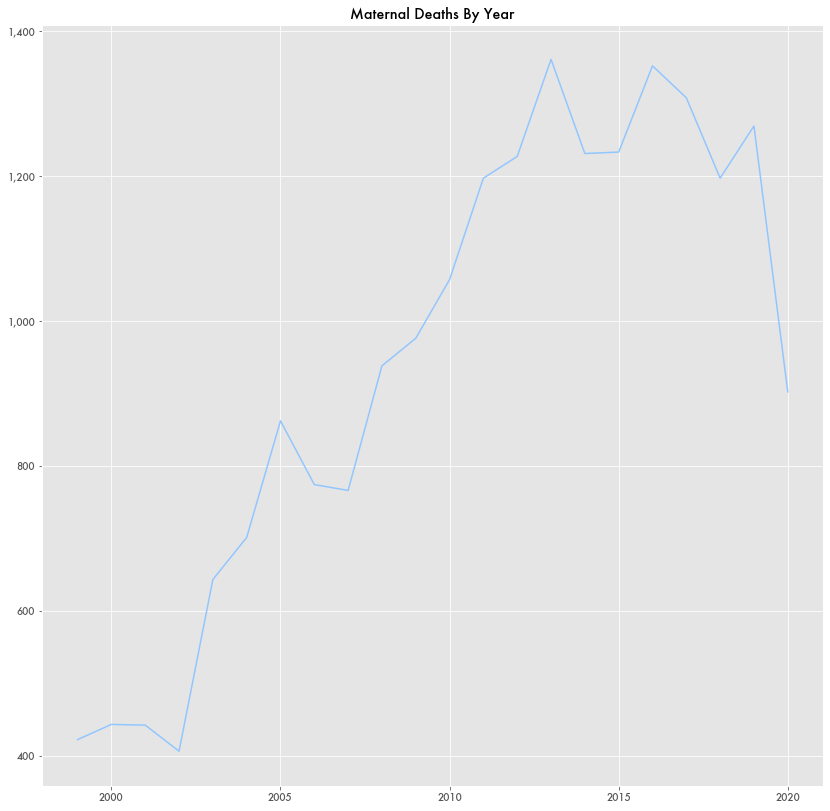
Not only was it unique that the maternal mortality rate was high, but it continues to increase over time despite being in steady decline through the 1990s according to a 2007 Centers for Disease Control (CDC) report.
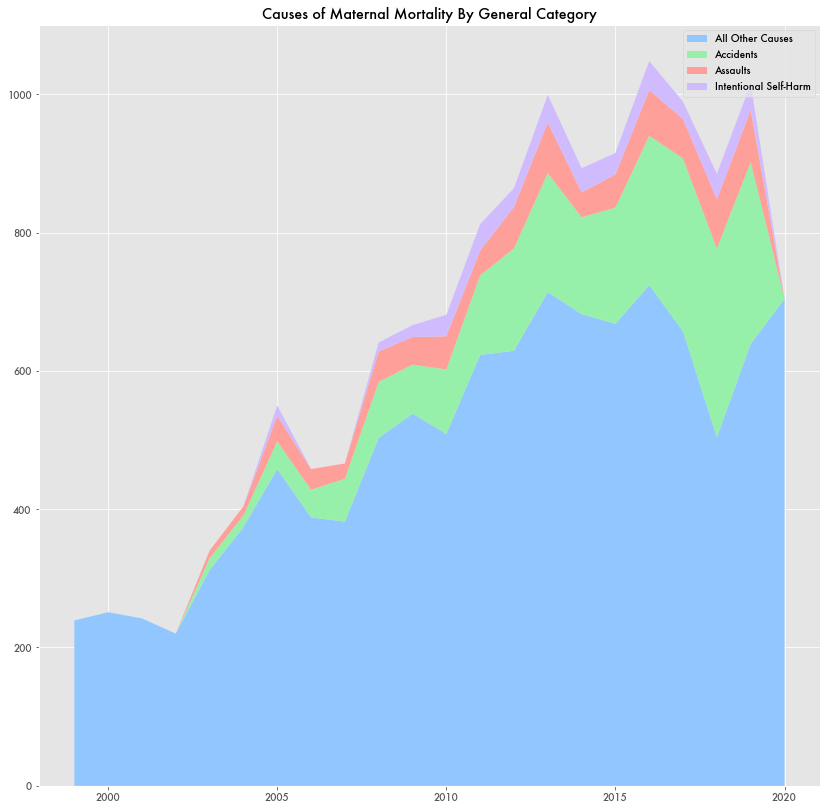
But during the pandemic, the maternal mortality rate took a sharp turn downward as assaults, accidents, and self-harm by recently pregnant mothers disappeared in 2020 based on CDC data.
While the changes could be a benefit of pandemic restrictions, the CDC has also recently implemented changes to account for large errors in reporting pregnancy-related mortality.
Non-disease related causes like overdoses have been a known issue for maternal mortality for some time now. A 2020 Commonwealth Fund report noted that mental health issues including substance abuse and suicide were among the leading causes of maternal mortality in the postpartum period alongside cardiomyopathy (weakened heart muscle). Hemorrhage and cardiovascular conditions are the most common causes during pregnancy, and infection is the leading cause during birth.
The high mortality rate is distinctly high among the African American population. The Commonwealth Fund noted that it is “more common among Black mothers with a college education than they are among white mothers with less than a high school education (40.2 vs. 25.0).”
A 2015 report from the Wilson Center also highlighted the common issue of substance abuse and maternal mortality:
In a review of all maternal deaths in the greater Philadelphia area from 2010 to 2012 that Begleiter participated in, she said reviewers found in all cases, “women had substance abuse problems and had multiple experiences with treatment.” Some were under child welfare supervision as children and as mothers, and a majority also exhibited behavioral issues.
Pre-Pandemic Decline Similar to Other Mortality Causes
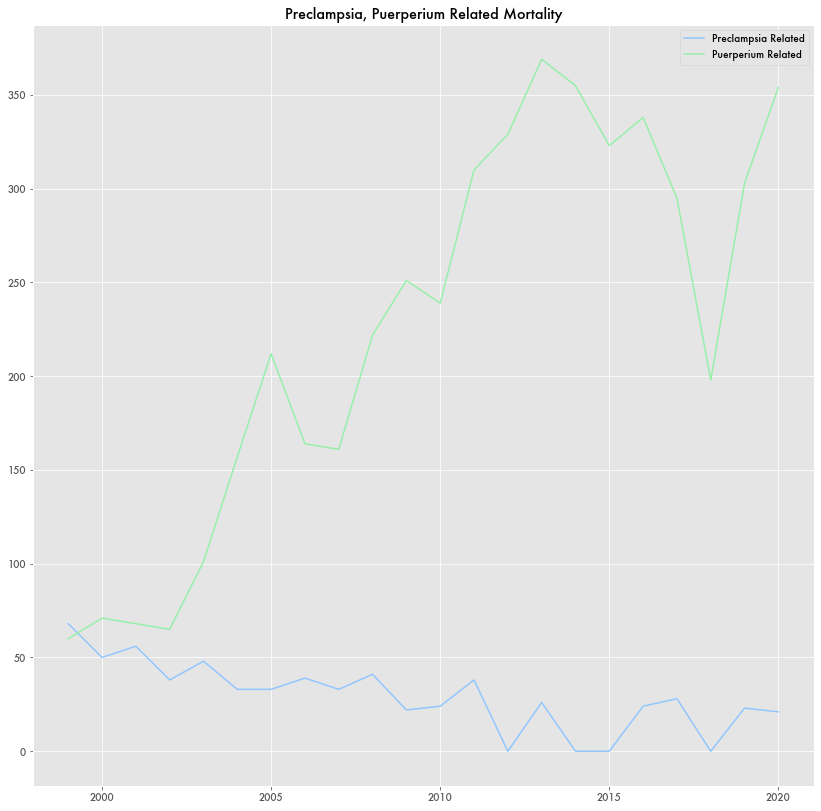
While external causes swung downward during the pandemic, other causes dropped pre-pandemic. This includes a range of causes connected to the puerperium, or postpartum, period. Maybe the largest category of maternal death independent of specific cause, these deaths went from over 350 a year in 2013 to 200 in 2018.
As Investigative Economics previously highlighted, a wide range of causes of mortality saw sharp drops around 2018 only to swing back to where they were in 2020.
Potential Errors
All CDC mortality data comes with caveats as to how the data is reported and reporting codes change regularly change over time.
But maternal mortality data may be unique in that pregnancy false-positive errors with respect to pregnancy have sometimes been reported as high as 50 percent and higher according to a 2017 CDC report.
According to one analysis, the number of reported decedents could be anomalously large and of an age that would make pregnancy unlikely.
797 deaths of women aged 40 and over had a checkbox entry indicating they were pregnant at the time of death or pregnant in the last year from any cause; 652 of these pregnancies were reported as occurring among those aged 45 and over; and 147 of these pregnancies were reported as occurring over age 85.
In 2018, the reporting method changed to account for these errors and move away from the “checkbox method”—where the reporter simply checked a box to indicate if the decedent was pregnant. The new method also eliminated the option if the decedent was over 45.
As a result, the maternal mortality rate would drop by 6 percent for the non-hispanic black population and less so for other populations.