Nursing Home Deaths Now Far Below Average
Nursing homes have been at the center of the COVID pandemic as the disease largely affects elderly populations. Since the end of May, over 65,000 deaths due to COVID-19 were reported from nursing homes in Centers for Disease Control (CDC) data.
The American Association of Retired Persons (AARP) estimates that 40 percent of all COVID deaths were in nursing homes, and the result could be protracted lawsuits, increased regulation of the industry, and there could be new changes in Medicaid to account for higher reimbursement for COVID patients. As a result, the CDC put out specific guidance for nursing homes which it considers to be at high-risk for COVID-19.
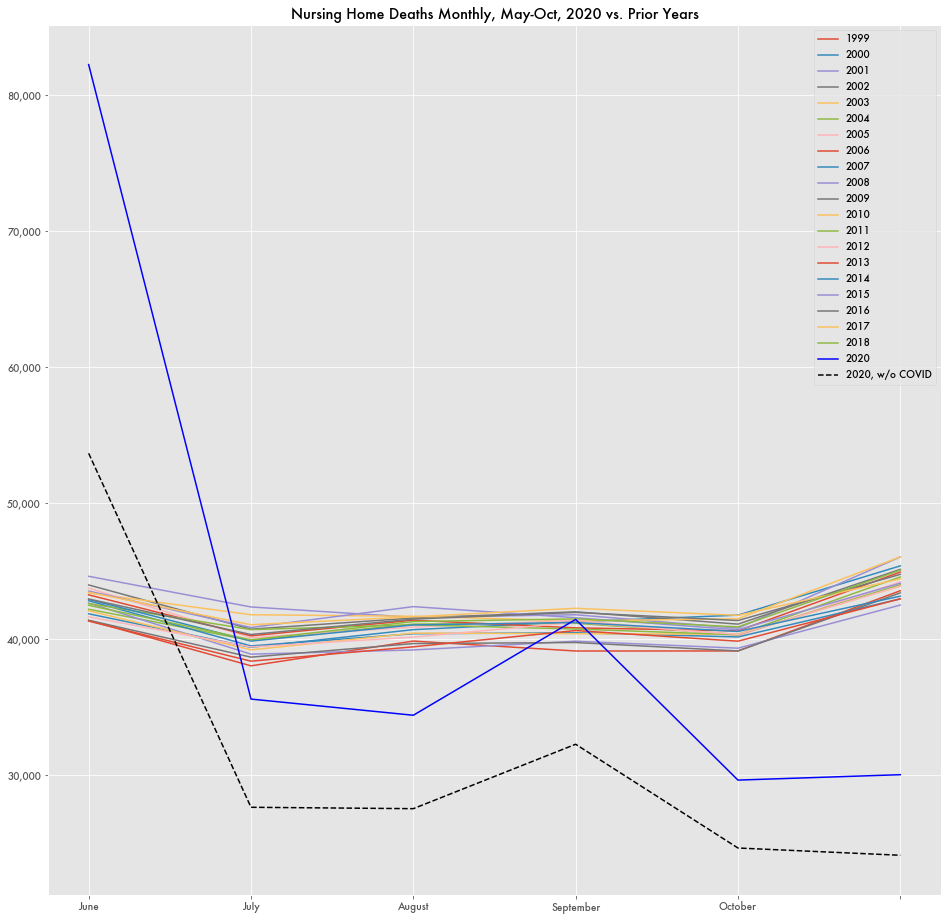
The CDC lists 82,239 nursing home deaths in the last week of May alone. That is far above the total number of nursing home deaths in a single month ever previously recorded in publicly available CDC data (1998-2018). It's over double the total death count for any other month in 2020 since then (the 2020 data does not include reporting before May 24th).
Yet, the large number of deaths in May appears as an anomaly in the CDC data. Since then, total monthly deaths in nursing homes have been substantially below the average for the last twenty years.
In September of this year, there were 10,000 fewer deaths in nursing homes than of any year prior. Without COVID-19 deaths included, there were 15,000 fewer deaths in September than previous averages.
The numbers indicate that COVID-19 is no longer driving a wave of mortality in nursing homes as it was in May or there are other effects of the lockdown affecting nursing home populations.
CDC’s Inconsistent Data
There could also be issues with CDC mortality data and how it is reported. Investigative Economics previously highlighted how preliminary mortality estimates showed a significantly lower total death rate trending for 2020 back in April.
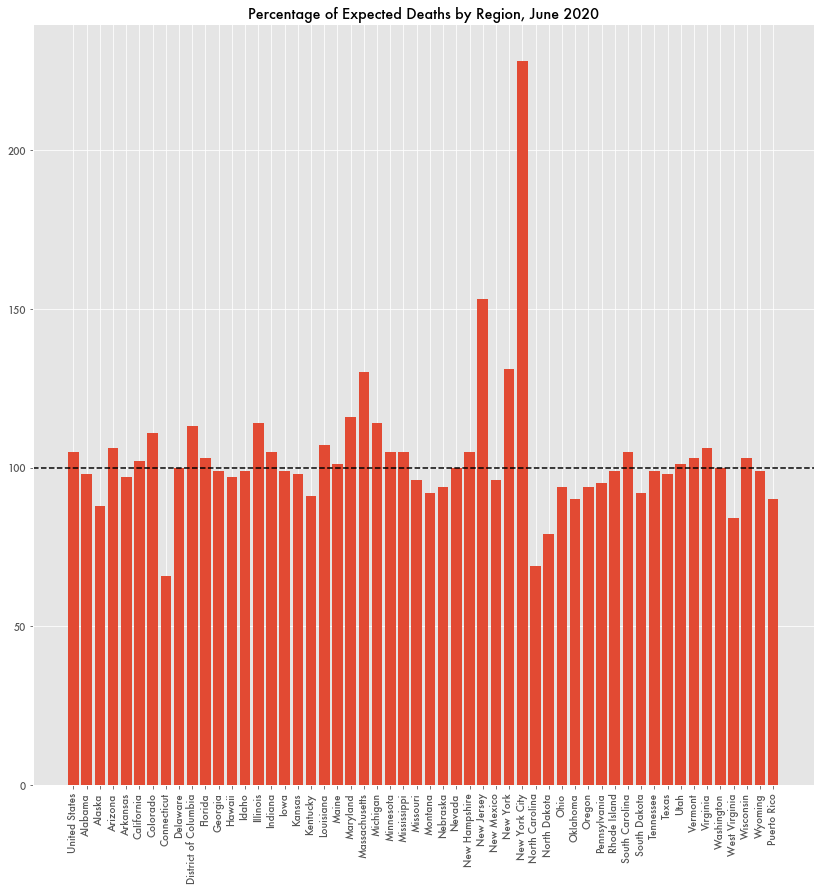
The CDC has since revised the numbers and the excess mortality rate for the U.S. is now higher than previous years, but at times that data showed certain states with a substantially low excess mortality rate.
Mainly rural states like Alaska and North Dakota, but also Connecticut, North Carolina, and Kentucky and others had expected death percentages in the 90s, 80s, or 70s at different times.
Those states also had incomplete reporting data in June. If those states were at 100 percent reporting, it would have meant significantly more deaths, which would also have pushed total U.S. mortality rates much higher—by about an additional 30,000 based on previous mortality rates.
Since then those numbers have changed significantly.
Occupancy Fluctuation
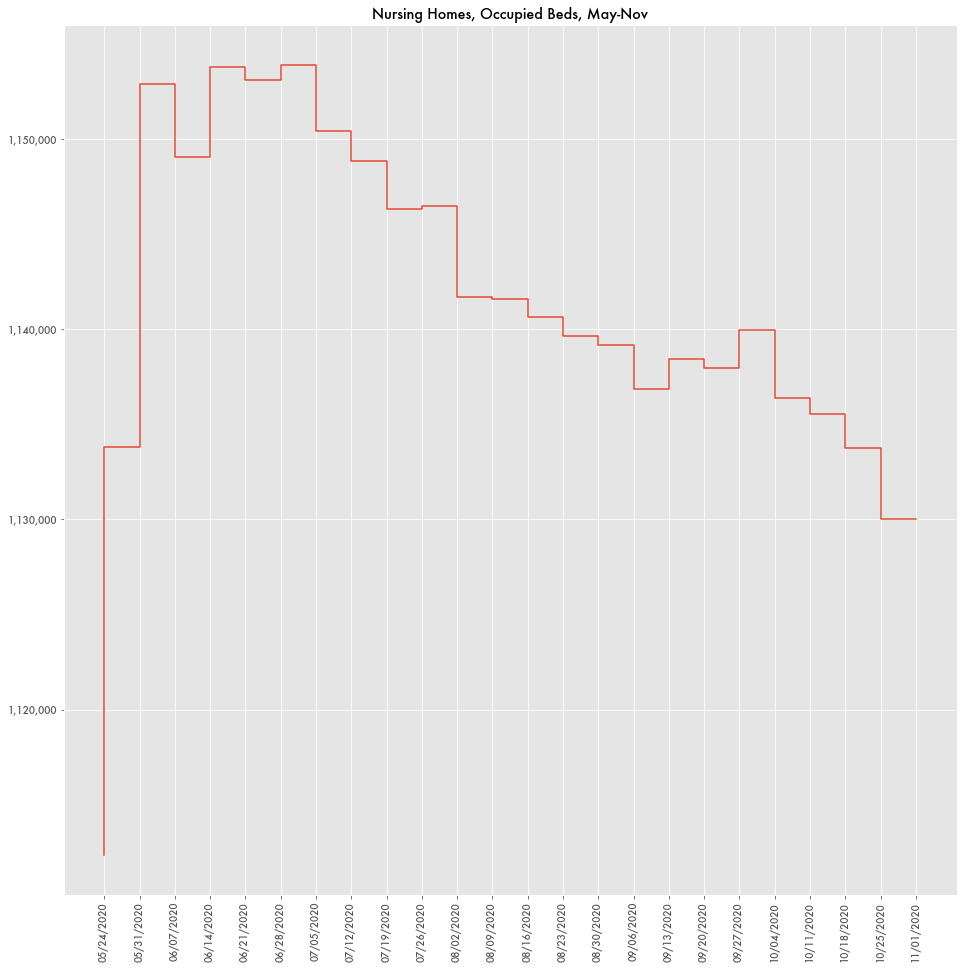
Besides the large spike in deaths in May, the number of nursing home residents has fluctuated dramatically. Total occupied beds spiked in May, but have since declined steadily, either as occupants leave nursing homes or as a remnant of how data is reported to the CDC.
In March, New York Governor Cuomo set an order that nursing homes could not prevent admission of patients with COVID that may have led to the spike in occupancy, but the governor has since denied the order being responsible for the large number of deaths in those facilities.